About Me
Dr. Weintraub's approach emphasizes collaboration and tailored treatment plans, ensuring patients receive the best possible care suited to their unique needs. He specializes in managing patients with a wide range of endocrine conditions, including obesity, diabetes, osteoporosis, and disorders of the thyroid, adrenal, and pituitary.
His particular interest lies in obesity medicine, a dynamic field that offers increasingly effective tools for treating and preventing weight gain, which is often the root cause of many chronic diseases. By working closely with nutritionists, surgeons, and other specialists, he strives to deliver holistic and effective care.
In addition to caring for patients, Dr. Weintraub is passionate about academic medicine, research, and training the next generation of physicians. He co-chairs the pharmacologic management of obesity guideline update through the Endocrine Society and serves on the exam writing committee for the American Board of Obesity Medicine. He is actively involved in clinical research within endocrinology and obesity medicine.
Academic & Professional Contributions

NEJM Course Faculty Director
Faculty Director for the New England Journal of Medicine Group's "Advancing Obesity Care" course, collaborating with leading experts to deliver evidence-based approaches for obesity management and GLP-1 therapies.
Learn More
Endocrine Society Guidelines Co-Chair
Co-Chair of the pharmacologic management of obesity guideline update through the Endocrine Society, leading the development of evidence-based recommendations for obesity pharmacotherapy.
Learn More
American Board of Obesity Medicine
Serving on the exam writing committee for the American Board of Obesity Medicine, contributing to the certification and education of obesity medicine specialists nationwide.
Learn More
Endocrine News Podcast
Featured expert discussing compounded obesity medications, addressing regulatory considerations, safety, efficacy, and patient access concerns in the evolving landscape of obesity pharmacotherapy.
Listen Now
DocWire News: EASO Framework Discussion
Expert commentary on how the European Association for the Study of Obesity framework reshapes clinical practice by moving beyond BMI to focus on individualized, health-centered approaches.
Watch VideoMedscape: GLP-1 Discontinuation Research
Discussing real-world data presented at ObesityWeek on weight regain patterns after GLP-1 discontinuation and implications for long-term obesity management strategies.
Read Article
ObesityWeek 2025
Presented real-world evidence on weight regain after GLP-1 discontinuation, highlighting the chronic nature of obesity and the importance of continuous treatment strategies.
View Details
2026 Columbia Cornell Obesity Medicine Course
Lecturer for the Columbia Cornell intensive CME program covering evidence-based approaches to obesity etiology, prevention, and treatment. Course emphasizes practical pharmacologic, nutritional, behavioral, and procedural interventions for patient-centered care.
Course Information
Endocrine Society Obesity Fellows Program Keynote
Recurring keynote speaker (2023, 2024, 2025) for the Endocrine Society’s Obesity Fellows Program, delivering the annual lecture on the state of obesity medicine to fellows training in the field nationwide.
Learn MoreAvailable for CME courses, grand rounds, and media interviews.
Request Speaking EngagementEducation and Training
-
Fellowship — Endocrinology, Diabetes & Metabolism
Cornell NewYork-Presbyterian HospitalMemorial Sloan Kettering Cancer Center -
Residency — Internal Medicine
Thomas Jefferson University Hospital -
Medical School
Rutgers Robert Wood Johnson Medical School -
Undergraduate
University of PennsylvaniaThe Wharton School
Practice Location
NYU Langone Diabetes & Endocrine Associates
222 East 41st Street, 23rd Floor
New York, NY 10017
Select Publications
Defining disease or delaying care? A conceptual and clinical appraisal of the Lancet obesity framework
Five-year weight loss maintenance with obesity pharmacotherapy
GLP-1 Receptor Agonist Outcomes, Safety, and Body Mass Index Change in a National Cohort of Patients on Dialysis
GLP-1 Receptor Agonists in Kidney Transplant Recipients with Pre-Existing Diabetes: A Retrospective Cohort Study
Sodium-Glucose Cotransporter-2 Inhibitors for Hyperglycemia in Phosphoinositide 3-kinase Pathway Inhibition
Recent Commentary
I actively share research insights, clinical commentary, and updates on obesity medicine and GLP-1 therapies across professional platforms.
FDA Approves Setmelanotide for Hypothalamic Obesity
Setmelanotide, an MC4R agonist, becomes the first FDA-approved treatment for hypothalamic obesity. Already approved for rare genetic forms of obesity involving the MC4R pathway, setmelanotide demonstrated 18.4% BMI reduction in the TRANSCEND trial of acquired hypothalamic obesity. This represents a valuable therapeutic option for a rare condition where conventional therapies have limited effectiveness.
View ThreadOral Agents, Lean Mass, and Long-term Therapy: Expert Discussion
In this final interview segment with Michael Nauck, MD, we explore practical implementation of oral semaglutide and orforglipron, addressing everyday dosing challenges and missed-dose protocols. We discuss interpreting lean mass shifts and the importance of long-term treatment planning as new GLP-1 therapies enter clinical practice.
Watch InterviewReduced GLP-1 Dosing Frequency Maintains Weight Loss
Patients who reduced GLP-1 dosing frequency from weekly to every other week successfully maintained weight loss and metabolic syndrome improvements in this case series. Findings suggest that while substantial GLP-1 level increases may be necessary to induce weight loss, more modest elevations may be sufficient for maintenance.
View ThreadPeptides With Real Evidence vs. The Hype
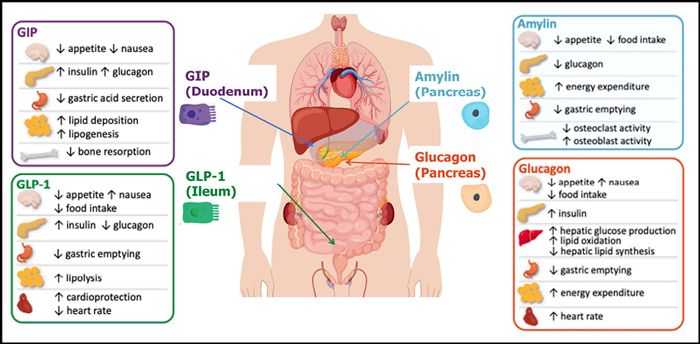
GLP-1 is just one of several nutrient-stimulated hormones with real human-trial data behind them. This post flags where the clinical evidence actually exists — amylin, GIP and glucagon agonism — and cautions against the rapidly growing market of peptides sold online without supporting trials or oversight.
Read Full PostFollow for Regular Updates
Join me for regular insights on obesity medicine, GLP-1 research, and endocrinology